 
One solution for atrial latency would be to programme dual-chamber antibradycardia pacing (DDD) with extended fixed AV delays. 
Taking atrial latency into consideration when programming AV delays is imperative. How should this patient’s device be programmed to avoid ventricular pacing?ĭDD = Dual-chamber antibradycardia pacing, AAI = Atrial demand pacing, VVI = Ventricular demand pacing. The generator was also replaced during this procedure (Assurity TM, Abbott). Atrial latency was still present with a much-improved pacing threshold ms). During the procedure the right atrial appendage was the only viable location. The patient was scheduled for an atrial lead reposition to restore AV synchrony. 
2 In this case study, ablation and subsequent fibrotic processes proximal to the lead tip are the probable causes of the conduction delay and eventual loss of capture. 1 It is important, particularly for patients with ventricular pacing indications, to consider atrial latency when programming the pacing mode and optimal AV delays. Typically, such delays occur due to significant scarring which slows conduction in the immediate vicinity of the pacing lead. The presence of an under sensed atrial arrhythmia with high grade AV block is possible, however her atrial tachycardias had previously demonstrated reasonable AV conduction so this was also unlikely (Figure 3).Ītrial latency can be described as a delay between atrial pacing stimulation and surface ECG p waves. Following every atrial paced event, p waves are not apparent on the surface ECG which suggests loss of atrial capture and effectively rules out complete heart block and further atrial latency. The atrial threshold test demonstrates loss of atrial capture. The most likely cause of heart failure decompensation in this case is loss of AV synchrony. What is the most likely cause of the heart failure decompensation based upon this pacing follow-up? The atrial threshold test can be seen in Figure 2.įigure 2: March 2021 Atrial Threshold TestĪ: Device EGMs with lead II, B: 12-lead ECG. On interrogation, no arrhythmia episodes had been recorded and RV thresholds were normal. Despite a high dose IV with furosemide, weight loss plateaued prompting a device check. The device was programmed DDDR 60 BPM with 100% atrial pacing and approximately 90% ventricular pacing.įigure 1: January 2019 Atrial Threshold TestĬlinically she had evidence of fluid overload and clinical heart failure with >10 kg recent weight gain. Otherwise, pacing checks had been normal with no further arrhythmic events. Since the ablation in 2015, the atrial threshold had been chronically elevated ms) with evidence of atrial latency ( Figure 1). During this procedure, a focal AT was identified proximal to the position of the right atrial pacing lead and ablated. A third ablation was performed in 2015 for symptomatic atrial tachycardia (AT). In 2013, she had a surgical atrial septal defect (ASD) closure and bi-atrial dilation had been seen on echocardiography. She had a dual chamber pacemaker in situ (Proponent TM, Boston Scientific) which was implanted in 2012, following periods of sinus arrest, following a redo typical atrial flutter ablation. Royal Brompton Hospital, Guys and St Thomas’ NHS Foundation TrustĪ 75-year-old female was admitted to hospital in March 2021 with a suspected acute heart failure decompensation. However, not seeing pacer spikes can be normal, such as when the patient's heart is beating faster than the rate set on the pacemaker.Jonathan Behar, MBBS PhD MRCP CCDS CEPS FEHRA You'll need a chest X-ray to rule out a fractured lead wire. If oversensing is the likely cause of the failure to pace, lower the mV on the sensitivity dial, as it raises the sensitivity of the pacemaker, and remove items that could cause electromechanical interference such as electric razors, radios, or cautery devices. 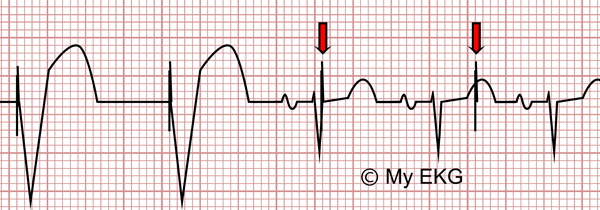
A pacemaker will sense, or pick up and interpret, muscle movement and artifact as heart beats if the sensitivity threshold is set too high, or there are items in the vicinity of the pacemaker that interfere with its signals, or the lead wire is fractured. If you're still not seeing pacer spikes it may mean the pacemaker is oversensing. (A good rule of thumb is to replace them every two to three days.) Then, check to make sure all connections are tight. Always check the batteries and replace them if necessary. Failure to pace is confirmed when there's no pacer spikes shown on your EKG or telemetry strip. Multiple causes including oversensing, wire fracture, lead displacement, or interference.Results in decreased or absent pacemaker function.Output failure occurs when a paced stimulus is not generated in a situation where expected. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
